Certified Medical Billers for Healthcare Practices Near You
Medical Billing Services For Small & Large Practices in USA
Ready to transform your practice's financial health? Our professional medical billing services take the stress out of claims processing. Whether you're running a small practice or large hospital, we help you boost revenue and minimize rejections. Let us handle the billing complexities while you focus on what you do best – caring for your patients.
Request A Free Quote
Take Control of Your Revenue Cycle
Running a healthcare practice is challenging enough without worrying about billing. As your all in one medical billing experts, our certified medical billers bring clarity to your revenue cycle management. Our team knows the ins and outs of medical billing for both small and large practices, ensuring you get paid what you deserve. We tackle the paperwork, chase down denials, and speed up payments – all so you can spend more time with your patients!
Outsource Billing for Health Practices
Strategic Medical Billing and Coding Services
MedLife is your strategic partner in medical billing services. We don’t just process claims; we optimize your entire revenue cycle. Our approach to medical coding for health practices combines accuracy with efficiency, helping you minimize denials and maximize revenue. We’ve streamlined everything from insurance eligibility verification to payment collection, empowering you to deliver outstanding patient care. Here’s how we help:
- Enrollment Verification
- Coding and Documentation
- Claim Submission
- Patient Communication
- Reimbursement and Follow-Up
- Technology Integration

17+ Years Experience
Our ultimate goal is to support our clients in reaching a state of financial stability and achieving excellence in their healthcare practices.
![{"type":"elementor","siteurl":"https://medlifembs.com/wp-json/","elements":[{"id":"4a1ba61","elType":"widget","isInner":false,"isLocked":false,"settings":{"image":{"id":5349,"url":"https://medlifembs.com/wp-content/uploads/2024/08/2cae958ec94a902c993819000abfca92.webp","alt":"Benefits of medical billing","source":"library","size":""},"sina_is_morphing_animation":"","sina_is_morphing_pattern":"yes","_animation":"fadeInLeft","pa_condition_repeater":[],"premium_tooltip_text":"Hi, I'm a global tooltip.","premium_tooltip_position":"top,bottom","width":{"unit":"px","size":"","sizes":[]},"width_tablet":{"unit":"px","size":"","sizes":[]},"width_mobile":{"unit":"px","size":"","sizes":[]},"height":{"unit":"px","size":430,"sizes":[]},"hover_animation":"grow","height_mobile":{"unit":"px","size":277,"sizes":[]},"image_border_radius":{"unit":"px","top":"0","right":"0","bottom":"0","left":"0","isLinked":true},"__globals__":{"image_border_color":"globals/colors?id=astglobalcolor5"},"image_size":"full","_transform_scale_popover_hover":"transform","_transform_scale_effect_hover_mobile":{"unit":"px","size":0.9,"sizes":[]},"_transform_scale_effect_hover":{"unit":"px","size":0.9,"sizes":[]},"_border_radius":{"unit":"px","top":"15","right":"15","bottom":"15","left":"15","isLinked":true},"image_custom_dimension":{"width":"","height":""},"caption_source":"none","caption":"","link_to":"none","link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"open_lightbox":"default","align":"","align_tablet":"","align_mobile":"","space":{"unit":"%","size":"","sizes":[]},"space_tablet":{"unit":"%","size":"","sizes":[]},"space_mobile":{"unit":"%","size":"","sizes":[]},"height_tablet":{"unit":"px","size":"","sizes":[]},"object-fit":"","object-fit_tablet":"","object-fit_mobile":"","object-position":"center center","object-position_tablet":"","object-position_mobile":"","opacity":{"unit":"px","size":"","sizes":[]},"css_filters_css_filter":"","css_filters_blur":{"unit":"px","size":0,"sizes":[]},"css_filters_brightness":{"unit":"px","size":100,"sizes":[]},"css_filters_contrast":{"unit":"px","size":100,"sizes":[]},"css_filters_saturate":{"unit":"px","size":100,"sizes":[]},"css_filters_hue":{"unit":"px","size":0,"sizes":[]},"opacity_hover":{"unit":"px","size":"","sizes":[]},"css_filters_hover_css_filter":"","css_filters_hover_blur":{"unit":"px","size":0,"sizes":[]},"css_filters_hover_brightness":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_contrast":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_saturate":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_hue":{"unit":"px","size":0,"sizes":[]},"background_hover_transition":{"unit":"px","size":"","sizes":[]},"image_border_border":"","image_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_color":"","image_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_box_shadow_box_shadow_type":"","image_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"caption_align":"","caption_align_tablet":"","caption_align_mobile":"","text_color":"","caption_background_color":"","caption_typography_typography":"","caption_typography_font_family":"","caption_typography_font_size":{"unit":"px","size":"","sizes":[]},"caption_typography_font_size_tablet":{"unit":"px","size":"","sizes":[]},"caption_typography_font_size_mobile":{"unit":"px","size":"","sizes":[]},"caption_typography_font_weight":"","caption_typography_text_transform":"","caption_typography_font_style":"","caption_typography_text_decoration":"","caption_typography_line_height":{"unit":"px","size":"","sizes":[]},"caption_typography_line_height_tablet":{"unit":"em","size":"","sizes":[]},"caption_typography_line_height_mobile":{"unit":"em","size":"","sizes":[]},"caption_typography_letter_spacing":{"unit":"px","size":"","sizes":[]},"caption_typography_letter_spacing_tablet":{"unit":"px","size":"","sizes":[]},"caption_typography_letter_spacing_mobile":{"unit":"px","size":"","sizes":[]},"caption_typography_word_spacing":{"unit":"px","size":"","sizes":[]},"caption_typography_word_spacing_tablet":{"unit":"em","size":"","sizes":[]},"caption_typography_word_spacing_mobile":{"unit":"em","size":"","sizes":[]},"caption_text_shadow_text_shadow_type":"","caption_text_shadow_text_shadow":{"horizontal":0,"vertical":0,"blur":10,"color":"rgba(0,0,0,0.3)"},"caption_space":{"unit":"px","size":"","sizes":[]},"caption_space_tablet":{"unit":"px","size":"","sizes":[]},"caption_space_mobile":{"unit":"px","size":"","sizes":[]},"_title":"","_margin":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_margin_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_margin_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_element_width":"","_element_width_tablet":"","_element_width_mobile":"","_element_custom_width":{"unit":"%","size":"","sizes":[]},"_element_custom_width_tablet":{"unit":"px","size":"","sizes":[]},"_element_custom_width_mobile":{"unit":"px","size":"","sizes":[]},"_flex_align_self":"","_flex_align_self_tablet":"","_flex_align_self_mobile":"","_flex_order":"","_flex_order_tablet":"","_flex_order_mobile":"","_flex_order_custom":"","_flex_order_custom_tablet":"","_flex_order_custom_mobile":"","_flex_size":"","_flex_size_tablet":"","_flex_size_mobile":"","_flex_grow":1,"_flex_grow_tablet":"","_flex_grow_mobile":"","_flex_shrink":1,"_flex_shrink_tablet":"","_flex_shrink_mobile":"","_element_vertical_align":"","_element_vertical_align_tablet":"","_element_vertical_align_mobile":"","_position":"","_offset_orientation_h":"start","_offset_x":{"unit":"px","size":0,"sizes":[]},"_offset_x_tablet":{"unit":"px","size":"","sizes":[]},"_offset_x_mobile":{"unit":"px","size":"","sizes":[]},"_offset_x_end":{"unit":"px","size":0,"sizes":[]},"_offset_x_end_tablet":{"unit":"px","size":"","sizes":[]},"_offset_x_end_mobile":{"unit":"px","size":"","sizes":[]},"_offset_orientation_v":"start","_offset_y":{"unit":"px","size":0,"sizes":[]},"_offset_y_tablet":{"unit":"px","size":"","sizes":[]},"_offset_y_mobile":{"unit":"px","size":"","sizes":[]},"_offset_y_end":{"unit":"px","size":0,"sizes":[]},"_offset_y_end_tablet":{"unit":"px","size":"","sizes":[]},"_offset_y_end_mobile":{"unit":"px","size":"","sizes":[]},"_z_index":"","_z_index_tablet":"","_z_index_mobile":"","_element_id":"","_css_classes":"","e_display_conditions":"","eael_wrapper_link_switch":"","eael_wrapper_link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"eael_hover_effect_switch":"","eael_hover_effect_enable_live_changes":"","eael_hover_effect_opacity_popover":"","eael_hover_effect_opacity":{"unit":"px","size":0.8,"sizes":[]},"eael_hover_effect_filter_popover":"","eael_hover_effect_blur_is_on":"","eael_hover_effect_blur":{"unit":"px","size":1,"sizes":[]},"eael_hover_effect_contrast_is_on":"","eael_hover_effect_contrast":{"unit":"px","size":80,"sizes":[]},"eael_hover_effect_grayscale_is_on":"","eael_hover_effect_grayscal":{"unit":"px","size":40,"sizes":[]},"eael_hover_effect_invert_is_on":"","eael_hover_effect_invert":{"unit":"px","size":70,"sizes":[]},"eael_hover_effect_saturate_is_on":"","eael_hover_effect_saturate":{"unit":"px","size":50,"sizes":[]},"eael_hover_effect_sepia_is_on":"","eael_hover_effect_sepia":{"unit":"px","size":50,"sizes":[]},"eael_hover_effect_offset_popover":"","eael_hover_effect_offset_left":{"unit":"px","size":5,"sizes":[]},"eael_hover_effect_offset_left_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_offset_left_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_offset_top":{"unit":"px","size":5,"sizes":[]},"eael_hover_effect_offset_top_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_offset_top_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_popover":"","eael_hover_effect_rotate_is_on":"","eael_hover_effect_transform_rotatex":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_transform_rotatex_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_rotatex_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_rotatey":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_transform_rotatey_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_rotatey_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_rotatez":{"unit":"px","size":5,"sizes":[]},"eael_hover_effect_transform_rotatez_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_rotatez_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_scale_is_on":"","eael_hover_effect_transform_scalex":{"unit":"px","size":0.9,"sizes":[]},"eael_hover_effect_transform_scalex_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_scalex_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_scaley":{"unit":"px","size":0.9,"sizes":[]},"eael_hover_effect_transform_scaley_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_scaley_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_skew_is_on":"","eael_hover_effect_transform_skewx":{"unit":"px","size":5,"sizes":[]},"eael_hover_effect_transform_skewx_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_skewx_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_skewy":{"unit":"px","size":5,"sizes":[]},"eael_hover_effect_transform_skewy_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_skewy_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_general_settings_duration":{"unit":"px","size":1000,"sizes":[]},"eael_hover_effect_general_settings_delay":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_general_settings_easing":"ease","eael_hover_effect_opacity_popover_hover":"","eael_hover_effect_opacity_hover":{"unit":"px","size":1,"sizes":[]},"eael_hover_effect_filter_hover_popover":"","eael_hover_effect_blur_hover_is_on":"","eael_hover_effect_blur_hover":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_contrast_hover_is_on":"","eael_hover_effect_contrast_hover":{"unit":"%","size":100,"sizes":[]},"eael_hover_effect_grayscale_hover_is_on":"","eael_hover_effect_grayscal_hover":{"unit":"%","size":0,"sizes":[]},"eael_hover_effect_invert_hover_is_on":"","eael_hover_effect_invert_hover":{"unit":"%","size":0,"sizes":[]},"eael_hover_effect_saturate_hover_is_on":"","eael_hover_effect_saturate_hover":{"unit":"%","size":100,"sizes":[]},"eael_hover_effect_sepia_hover_is_on":"","eael_hover_effect_sepia_hover":{"unit":"px","size":1,"sizes":[]},"eael_hover_effect_offset_hover_popover":"","eael_hover_effect_offset_hover_left":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_offset_hover_left_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_offset_hover_left_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_offset_hover_top":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_offset_hover_top_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_offset_hover_top_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_popover":"","eael_hover_effect_rotate_hover_is_on":"","eael_hover_effect_transform_hover_rotatex":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_transform_hover_rotatex_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_rotatex_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_rotatey":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_transform_hover_rotatey_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_rotatey_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_rotatez":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_transform_hover_rotatez_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_rotatez_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_scale_hover_is_on":"","eael_hover_effect_transform_hover_scalex":{"unit":"px","size":1,"sizes":[]},"eael_hover_effect_transform_hover_scalex_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_scalex_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_scaley":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_transform_hover_scaley_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_scaley_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_skew_hover_is_on":"","eael_hover_effect_transform_hover_skewx":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_transform_hover_skewx_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_skewx_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_skewy":{"unit":"px","size":0,"sizes":[]},"eael_hover_effect_transform_hover_skewy_tablet":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_transform_hover_skewy_mobile":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_general_settings_hover_duration":{"unit":"px","size":1000,"sizes":[]},"eael_hover_effect_general_settings_hover_delay":{"unit":"px","size":"","sizes":[]},"eael_hover_effect_general_settings_hover_easing":"ease","eael_hover_effect_hover_tilt":"","pa_display_conditions_switcher":"","pa_display_action":"show","pa_display_when":"any","premium_fe_switcher":"","premium_fe_target":"","premium_fe_translate_switcher":"","premium_fe_Xtranslate":{"unit":"px","size":"","sizes":{"from":0,"to":5}},"premium_fe_Xtranslate_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Xtranslate_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_Ytranslate":{"unit":"px","size":"","sizes":{"from":0,"to":5}},"premium_fe_Ytranslate_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Ytranslate_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_trans_duration":{"unit":"px","size":1000,"sizes":[]},"premium_fe_trans_delay":{"unit":"px","size":"","sizes":[]},"premium_fe_rotate_switcher":"","premium_fe_Xrotate":{"unit":"deg","size":"","sizes":{"from":0,"to":45}},"premium_fe_Xrotate_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Xrotate_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_Yrotate":{"unit":"deg","size":"","sizes":{"from":0,"to":45}},"premium_fe_Yrotate_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Yrotate_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_Zrotate":{"unit":"deg","size":"","sizes":{"from":0,"to":45}},"premium_fe_Zrotate_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Zrotate_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_rotate_duration":{"unit":"px","size":1000,"sizes":[]},"premium_fe_rotate_delay":{"unit":"px","size":"","sizes":[]},"premium_fe_scale_switcher":"","premium_fe_Xscale":{"unit":"px","size":"","sizes":{"from":1,"to":1.2}},"premium_fe_Xscale_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Xscale_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_Yscale":{"unit":"px","size":"","sizes":{"from":1,"to":1.2}},"premium_fe_Yscale_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Yscale_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_scale_duration":{"unit":"px","size":1000,"sizes":[]},"premium_fe_scale_delay":{"unit":"px","size":"","sizes":[]},"premium_fe_skew_switcher":"","premium_fe_Xskew":{"unit":"deg","size":"","sizes":{"from":0,"to":20}},"premium_fe_Xskew_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Xskew_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_Yskew":{"unit":"deg","size":"","sizes":{"from":0,"to":20}},"premium_fe_Yskew_tablet":{"unit":"px","size":"","sizes":[]},"premium_fe_Yskew_mobile":{"unit":"px","size":"","sizes":[]},"premium_fe_skew_duration":{"unit":"px","size":1000,"sizes":[]},"premium_fe_skew_delay":{"unit":"px","size":"","sizes":[]},"premium_fe_opacity_switcher":"","premium_fe_bg_color_switcher":"","premium_fe_blur_switcher":"","premium_fe_contrast_switcher":"","premium_fe_gScale_switcher":"","premium_fe_hue_switcher":"","premium_fe_brightness_switcher":"","premium_fe_saturate_switcher":"","premium_fe_direction":"alternate","premium_fe_loop":"default","premium_fe_loop_number":3,"premium_fe_easing":"easeInOutSine","premium_fe_ease_step":5,"premium_fe_disable_safari":"","premium_tooltip_switcher":"","pa_tooltip_target":"","premium_tooltip_type":"text","premium_tooltip_icon_switcher":"","premium_tooltip_icon":{"value":"fas fa-star","library":"fa-solid"},"premium_tooltip_lottie_url":"","premium_tooltip_lottie_loop":"true","premium_tooltip_lottie_reverse":"","hide_tooltip_on":[],"premium_tooltip_text_color":"","premium_tooltip_text_typo_typography":"","premium_tooltip_text_typo_font_family":"","premium_tooltip_text_typo_font_size":{"unit":"px","size":"","sizes":[]},"premium_tooltip_text_typo_font_size_tablet":{"unit":"px","size":"","sizes":[]},"premium_tooltip_text_typo_font_size_mobile":{"unit":"px","size":"","sizes":[]},"premium_tooltip_text_typo_font_weight":"","premium_tooltip_text_typo_text_transform":"","premium_tooltip_text_typo_font_style":"","premium_tooltip_text_typo_text_decoration":"","premium_tooltip_text_typo_line_height":{"unit":"px","size":"","sizes":[]},"premium_tooltip_text_typo_line_height_tablet":{"unit":"em","size":"","sizes":[]},"premium_tooltip_text_typo_line_height_mobile":{"unit":"em","size":"","sizes":[]},"premium_tooltip_text_typo_letter_spacing":{"unit":"px","size":"","sizes":[]},"premium_tooltip_text_typo_letter_spacing_tablet":{"unit":"px","size":"","sizes":[]},"premium_tooltip_text_typo_letter_spacing_mobile":{"unit":"px","size":"","sizes":[]},"premium_tooltip_text_typo_word_spacing":{"unit":"px","size":"","sizes":[]},"premium_tooltip_text_typo_word_spacing_tablet":{"unit":"em","size":"","sizes":[]},"premium_tooltip_text_typo_word_spacing_mobile":{"unit":"em","size":"","sizes":[]},"premium_tooltip_text_shadow_text_shadow_type":"","premium_tooltip_text_shadow_text_shadow":{"horizontal":0,"vertical":0,"blur":10,"color":"rgba(0,0,0,0.3)"},"premium_tooltip_icon_color":"","premium_tooltip_icon_size":{"unit":"px","size":"","sizes":[]},"premium_tooltip_icon_size_tablet":{"unit":"px","size":"","sizes":[]},"premium_tooltip_icon_size_mobile":{"unit":"px","size":"","sizes":[]},"premium_tooltip_icon_shadow_text_shadow_type":"","premium_tooltip_icon_shadow_text_shadow":{"horizontal":0,"vertical":0,"blur":10,"color":"rgba(0,0,0,0.3)"},"premium_tooltip_img_size":{"unit":"px","size":100,"sizes":[]},"premium_tooltip_img_size_tablet":{"unit":"px","size":"","sizes":[]},"premium_tooltip_img_size_mobile":{"unit":"px","size":"","sizes":[]},"premium_tooltip_img_fit":"cover","premium_tooltip_img_fit_tablet":"","premium_tooltip_img_fit_mobile":"","premium_tooltip_container_bg_background":"","premium_tooltip_container_bg_color":"","premium_tooltip_container_bg_color_stop":{"unit":"%","size":0,"sizes":[]},"premium_tooltip_container_bg_color_stop_tablet":{"unit":"%","size":"","sizes":[]},"premium_tooltip_container_bg_color_stop_mobile":{"unit":"%","size":"","sizes":[]},"premium_tooltip_container_bg_color_b":"#f2295b","premium_tooltip_container_bg_color_b_stop":{"unit":"%","size":100,"sizes":[]},"premium_tooltip_container_bg_color_b_stop_tablet":{"unit":"%","size":"","sizes":[]},"premium_tooltip_container_bg_color_b_stop_mobile":{"unit":"%","size":"","sizes":[]},"premium_tooltip_container_bg_gradient_type":"linear","premium_tooltip_container_bg_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"premium_tooltip_container_bg_gradient_angle_tablet":{"unit":"deg","size":"","sizes":[]},"premium_tooltip_container_bg_gradient_angle_mobile":{"unit":"deg","size":"","sizes":[]},"premium_tooltip_container_bg_gradient_position":"center center","premium_tooltip_container_bg_gradient_position_tablet":"","premium_tooltip_container_bg_gradient_position_mobile":"","premium_tooltip_container_bg_image":{"url":"","id":"","size":""},"premium_tooltip_container_bg_image_tablet":{"url":"","id":"","size":""},"premium_tooltip_container_bg_image_mobile":{"url":"","id":"","size":""},"premium_tooltip_container_bg_position":"","premium_tooltip_container_bg_position_tablet":"","premium_tooltip_container_bg_position_mobile":"","premium_tooltip_container_bg_xpos":{"unit":"px","size":0,"sizes":[]},"premium_tooltip_container_bg_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"premium_tooltip_container_bg_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"premium_tooltip_container_bg_ypos":{"unit":"px","size":0,"sizes":[]},"premium_tooltip_container_bg_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"premium_tooltip_container_bg_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"premium_tooltip_container_bg_attachment":"","premium_tooltip_container_bg_repeat":"","premium_tooltip_container_bg_repeat_tablet":"","premium_tooltip_container_bg_repeat_mobile":"","premium_tooltip_container_bg_size":"","premium_tooltip_container_bg_size_tablet":"","premium_tooltip_container_bg_size_mobile":"","premium_tooltip_container_bg_bg_width":{"unit":"%","size":100,"sizes":[]},"premium_tooltip_container_bg_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"premium_tooltip_container_bg_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"premium_tooltip_container_bg_video_link":"","premium_tooltip_container_bg_video_start":"","premium_tooltip_container_bg_video_end":"","premium_tooltip_container_bg_play_once":"","premium_tooltip_container_bg_play_on_mobile":"","premium_tooltip_container_bg_privacy_mode":"","premium_tooltip_container_bg_video_fallback":{"url":"","id":"","size":""},"premium_tooltip_container_bg_slideshow_gallery":[],"premium_tooltip_container_bg_slideshow_loop":"yes","premium_tooltip_container_bg_slideshow_slide_duration":5000,"premium_tooltip_container_bg_slideshow_slide_transition":"fade","premium_tooltip_container_bg_slideshow_transition_duration":500,"premium_tooltip_container_bg_slideshow_background_size":"","premium_tooltip_container_bg_slideshow_background_size_tablet":"","premium_tooltip_container_bg_slideshow_background_size_mobile":"","premium_tooltip_container_bg_slideshow_background_position":"","premium_tooltip_container_bg_slideshow_background_position_tablet":"","premium_tooltip_container_bg_slideshow_background_position_mobile":"","premium_tooltip_container_bg_slideshow_lazyload":"","premium_tooltip_container_bg_slideshow_ken_burns":"","premium_tooltip_container_bg_slideshow_ken_burns_zoom_direction":"in","premium_tooltip_container_border_border":"","premium_tooltip_container_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"premium_tooltip_container_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"premium_tooltip_container_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"premium_tooltip_container_border_color":"","premium_tooltip_container_border_radius":{"unit":"px","size":"","sizes":[]},"premium_tooltip_container_box_shadow_box_shadow_type":"","premium_tooltip_container_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"premium_tooltip_container_box_shadow_box_shadow_position":" ","premium_tooltip_container_padding":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"premium_tooltip_container_padding_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"premium_tooltip_container_padding_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"premium_tooltip_arrow_color":"","premium_tooltip_mouse_follow":"","premium_tooltip_interactive":"yes","premium_tooltip_arrow":"","premium_tooltip_trigger":"hover","premium_tooltip_distance_position":6,"premium_tooltip_min_width":{"unit":"px","size":"","sizes":[]},"premium_tooltip_min_width_tablet":{"unit":"px","size":"","sizes":[]},"premium_tooltip_min_width_mobile":{"unit":"px","size":"","sizes":[]},"premium_tooltip_max_width":{"unit":"px","size":"","sizes":[]},"premium_tooltip_max_width_tablet":{"unit":"px","size":"","sizes":[]},"premium_tooltip_max_width_mobile":{"unit":"px","size":"","sizes":[]},"premium_tooltip_height":{"unit":"px","size":"","sizes":[]},"premium_tooltip_height_tablet":{"unit":"px","size":"","sizes":[]},"premium_tooltip_height_mobile":{"unit":"px","size":"","sizes":[]},"premium_tooltip_anime":"fade","premium_tooltip_anime_dur":350,"premium_tooltip_delay":10,"pa_tooltip_zindex":"","premium_wrapper_link_selection":"url","premium_wrapper_link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"premium_wrapper_existing_link":"","motion_fx_motion_fx_scrolling":"","motion_fx_translateY_effect":"","motion_fx_translateY_direction":"","motion_fx_translateY_speed":{"unit":"px","size":4,"sizes":[]},"motion_fx_translateY_affectedRange":{"unit":"%","size":"","sizes":{"start":0,"end":100}},"motion_fx_translateX_effect":"","motion_fx_translateX_direction":"","motion_fx_translateX_speed":{"unit":"px","size":4,"sizes":[]},"motion_fx_translateX_affectedRange":{"unit":"%","size":"","sizes":{"start":0,"end":100}},"motion_fx_opacity_effect":"","motion_fx_opacity_direction":"out-in","motion_fx_opacity_level":{"unit":"px","size":10,"sizes":[]},"motion_fx_opacity_range":{"unit":"%","size":"","sizes":{"start":20,"end":80}},"motion_fx_blur_effect":"","motion_fx_blur_direction":"out-in","motion_fx_blur_level":{"unit":"px","size":7,"sizes":[]},"motion_fx_blur_range":{"unit":"%","size":"","sizes":{"start":20,"end":80}},"motion_fx_rotateZ_effect":"","motion_fx_rotateZ_direction":"","motion_fx_rotateZ_speed":{"unit":"px","size":1,"sizes":[]},"motion_fx_rotateZ_affectedRange":{"unit":"%","size":"","sizes":{"start":0,"end":100}},"motion_fx_scale_effect":"","motion_fx_scale_direction":"out-in","motion_fx_scale_speed":{"unit":"px","size":4,"sizes":[]},"motion_fx_scale_range":{"unit":"%","size":"","sizes":{"start":20,"end":80}},"motion_fx_transform_origin_x":"center","motion_fx_transform_origin_y":"center","motion_fx_devices":["desktop","tablet","mobile"],"motion_fx_range":"","motion_fx_motion_fx_mouse":"","motion_fx_mouseTrack_effect":"","motion_fx_mouseTrack_direction":"","motion_fx_mouseTrack_speed":{"unit":"px","size":1,"sizes":[]},"motion_fx_tilt_effect":"","motion_fx_tilt_direction":"","motion_fx_tilt_speed":{"unit":"px","size":4,"sizes":[]},"sticky":"","sticky_on":["desktop","tablet","mobile"],"sticky_offset":0,"sticky_offset_tablet":"","sticky_offset_mobile":"","sticky_effects_offset":0,"sticky_effects_offset_tablet":"","sticky_effects_offset_mobile":"","sticky_parent":"","_animation_tablet":"","_animation_mobile":"","animation_duration":"","_animation_delay":"","_transform_rotate_popover":"","_transform_rotateZ_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateZ_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateZ_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotate_3d":"","_transform_rotateX_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateX_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateX_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateY_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_perspective_effect":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translate_popover":"","_transform_translateX_effect":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scale_popover":"","_transform_keep_proportions":"yes","_transform_scale_effect":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_skew_popover":"","_transform_skewX_effect":{"unit":"px","size":"","sizes":[]},"_transform_skewX_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewX_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect":{"unit":"px","size":"","sizes":[]},"_transform_skewY_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_flipX_effect":"","_transform_flipY_effect":"","_transform_rotate_popover_hover":"","_transform_rotateZ_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateZ_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateZ_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotate_3d_hover":"","_transform_rotateX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateX_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateX_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateY_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_perspective_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translate_popover_hover":"","_transform_translateX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_keep_proportions_hover":"yes","_transform_scale_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_skew_popover_hover":"","_transform_skewX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_skewX_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewX_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_skewY_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_flipX_effect_hover":"","_transform_flipY_effect_hover":"","_transform_transition_hover":{"unit":"px","size":"","sizes":[]},"motion_fx_transform_x_anchor_point":"","motion_fx_transform_x_anchor_point_tablet":"","motion_fx_transform_x_anchor_point_mobile":"","motion_fx_transform_y_anchor_point":"","motion_fx_transform_y_anchor_point_tablet":"","motion_fx_transform_y_anchor_point_mobile":"","_background_background":"","_background_color":"","_background_color_stop":{"unit":"%","size":0,"sizes":[]},"_background_color_stop_tablet":{"unit":"%","size":"","sizes":[]},"_background_color_stop_mobile":{"unit":"%","size":"","sizes":[]},"_background_color_b":"#f2295b","_background_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_background_color_b_stop_tablet":{"unit":"%","size":"","sizes":[]},"_background_color_b_stop_mobile":{"unit":"%","size":"","sizes":[]},"_background_gradient_type":"linear","_background_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_background_gradient_angle_tablet":{"unit":"deg","size":"","sizes":[]},"_background_gradient_angle_mobile":{"unit":"deg","size":"","sizes":[]},"_background_gradient_position":"center center","_background_gradient_position_tablet":"","_background_gradient_position_mobile":"","_background_image":{"url":"","id":"","size":""},"_background_image_tablet":{"url":"","id":"","size":""},"_background_image_mobile":{"url":"","id":"","size":""},"_background_position":"","_background_position_tablet":"","_background_position_mobile":"","_background_xpos":{"unit":"px","size":0,"sizes":[]},"_background_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_ypos":{"unit":"px","size":0,"sizes":[]},"_background_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_attachment":"","_background_repeat":"","_background_repeat_tablet":"","_background_repeat_mobile":"","_background_size":"","_background_size_tablet":"","_background_size_mobile":"","_background_bg_width":{"unit":"%","size":100,"sizes":[]},"_background_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_background_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_background_video_link":"","_background_video_start":"","_background_video_end":"","_background_play_once":"","_background_play_on_mobile":"","_background_privacy_mode":"","_background_video_fallback":{"url":"","id":"","size":""},"_background_slideshow_gallery":[],"_background_slideshow_loop":"yes","_background_slideshow_slide_duration":5000,"_background_slideshow_slide_transition":"fade","_background_slideshow_transition_duration":500,"_background_slideshow_background_size":"","_background_slideshow_background_size_tablet":"","_background_slideshow_background_size_mobile":"","_background_slideshow_background_position":"","_background_slideshow_background_position_tablet":"","_background_slideshow_background_position_mobile":"","_background_slideshow_lazyload":"","_background_slideshow_ken_burns":"","_background_slideshow_ken_burns_zoom_direction":"in","_background_hover_background":"","_background_hover_color":"","_background_hover_color_stop":{"unit":"%","size":0,"sizes":[]},"_background_hover_color_stop_tablet":{"unit":"%","size":"","sizes":[]},"_background_hover_color_stop_mobile":{"unit":"%","size":"","sizes":[]},"_background_hover_color_b":"#f2295b","_background_hover_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_background_hover_color_b_stop_tablet":{"unit":"%","size":"","sizes":[]},"_background_hover_color_b_stop_mobile":{"unit":"%","size":"","sizes":[]},"_background_hover_gradient_type":"linear","_background_hover_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_background_hover_gradient_angle_tablet":{"unit":"deg","size":"","sizes":[]},"_background_hover_gradient_angle_mobile":{"unit":"deg","size":"","sizes":[]},"_background_hover_gradient_position":"center center","_background_hover_gradient_position_tablet":"","_background_hover_gradient_position_mobile":"","_background_hover_image":{"url":"","id":"","size":""},"_background_hover_image_tablet":{"url":"","id":"","size":""},"_background_hover_image_mobile":{"url":"","id":"","size":""},"_background_hover_position":"","_background_hover_position_tablet":"","_background_hover_position_mobile":"","_background_hover_xpos":{"unit":"px","size":0,"sizes":[]},"_background_hover_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_hover_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_hover_attachment":"","_background_hover_repeat":"","_background_hover_repeat_tablet":"","_background_hover_repeat_mobile":"","_background_hover_size":"","_background_hover_size_tablet":"","_background_hover_size_mobile":"","_background_hover_bg_width":{"unit":"%","size":100,"sizes":[]},"_background_hover_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_background_hover_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_background_hover_video_link":"","_background_hover_video_start":"","_background_hover_video_end":"","_background_hover_play_once":"","_background_hover_play_on_mobile":"","_background_hover_privacy_mode":"","_background_hover_video_fallback":{"url":"","id":"","size":""},"_background_hover_slideshow_gallery":[],"_background_hover_slideshow_loop":"yes","_background_hover_slideshow_slide_duration":5000,"_background_hover_slideshow_slide_transition":"fade","_background_hover_slideshow_transition_duration":500,"_background_hover_slideshow_background_size":"","_background_hover_slideshow_background_size_tablet":"","_background_hover_slideshow_background_size_mobile":"","_background_hover_slideshow_background_position":"","_background_hover_slideshow_background_position_tablet":"","_background_hover_slideshow_background_position_mobile":"","_background_hover_slideshow_lazyload":"","_background_hover_slideshow_ken_burns":"","_background_hover_slideshow_ken_burns_zoom_direction":"in","_background_hover_transition":{"unit":"px","size":"","sizes":[]},"_border_border":"","_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_color":"","_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_box_shadow_box_shadow_type":"","_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"_box_shadow_box_shadow_position":" ","_border_hover_border":"","_border_hover_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_color":"","_border_radius_hover":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_hover_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_hover_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_box_shadow_hover_box_shadow_type":"","_box_shadow_hover_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"_box_shadow_hover_box_shadow_position":" ","_border_hover_transition":{"unit":"px","size":"","sizes":[]},"_mask_switch":"","_mask_shape":"circle","_mask_image":{"url":"","id":"","size":""},"_mask_notice":"","_mask_size":"contain","_mask_size_tablet":"","_mask_size_mobile":"","_mask_size_scale":{"unit":"%","size":100,"sizes":[]},"_mask_size_scale_tablet":{"unit":"px","size":"","sizes":[]},"_mask_size_scale_mobile":{"unit":"px","size":"","sizes":[]},"_mask_position":"center center","_mask_position_tablet":"","_mask_position_mobile":"","_mask_position_x":{"unit":"%","size":0,"sizes":[]},"_mask_position_x_tablet":{"unit":"px","size":"","sizes":[]},"_mask_position_x_mobile":{"unit":"px","size":"","sizes":[]},"_mask_position_y":{"unit":"%","size":0,"sizes":[]},"_mask_position_y_tablet":{"unit":"px","size":"","sizes":[]},"_mask_position_y_mobile":{"unit":"px","size":"","sizes":[]},"_mask_repeat":"no-repeat","_mask_repeat_tablet":"","_mask_repeat_mobile":"","hide_desktop":"","hide_tablet":"","hide_mobile":"","_attributes":"","custom_css":"","wpr_custom_css":""},"defaultEditSettings":{"defaultEditRoute":"content"},"elements":[],"widgetType":"image","htmlCache":"\t\t\n\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\n\t\t","editSettings":{"defaultEditRoute":"content","panel":{"activeTab":"content","activeSection":"section_image"}}}]}](https://medlifembs.com/wp-content/uploads/2025/01/Medical-Billing-Services-For-Small-Practices.png)
Medical Billing Services For Small Practices
Optimize your revenue cycle with our healthcare billing services for small practices, designed to ensure faster claims processing, improved cash flow, and more time to focus on patient care.
- Faster Claims: We get your claims processed quickly and correctly
- Better Cash Flow: Watch your revenue grow with improved accuracy
- Complete Support: From claims to detailed patient statement handling
- Expert Team: Real people using smart technology to solve billing challenges
- Focus on Patients: More time for care, less time on paperwork
- Clear Reporting: Stay informed with easy-to-understand performance updates
- Streamlined Revenue: Accounts receivable management that works
Ready to Boost Your Practice's Financial Health?
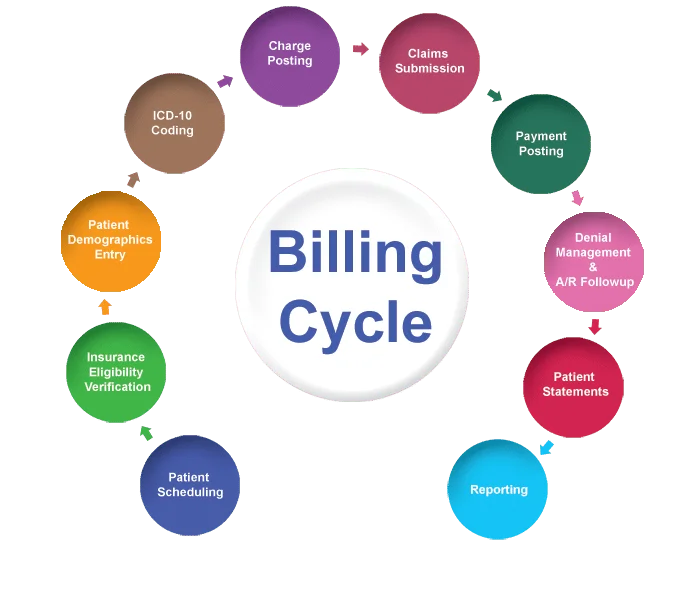
MedLife is your Dedicated Partner in Entire Billing Process
We know medical billing inside and out. Our team brings years of experience to every claim, using streamlined EDI enrollment and proven processes to get you paid faster. We’re thorough with:
- Detailed AR Reports: Track every dollar with clear, actionable insights
- Smart Appeals: Effective denial management that gets results
- Expert Negotiations: We advocate for your rightful reimbursement
-
Comprehensive Billing Solutions
-
Seamless Provider Enrollment
-
Reimbursement Processing
Medical Billing Solutions
Tired of complex billing processes? Our certified medical billers make it simple. We create custom solutions that fit your practice, whether you’re a small clinic or a large hospital. Let’s build a roadmap to your financial success with medical transcription solutions that work.
Seamless Provider Enrollment
Getting into insurance networks shouldn’t give you headaches. Our credentialing support makes it easier, handling everything from applications to contract negotiations. We’ll help you build a strong network that brings in more patients and revenue.
Hassle-Free Reimbursement Processing
Say goodbye to paperwork stress. Our experts handle CMS 1500 and UB-04 forms with precision, ensuring simplified out-of-network billing and faster payments. Trust us with your CMS paperwork while you focus on patient care.
Partner with a Team That Understands Your Needs
Looking for a medical billing company that truly gets it? That’s us. We combine skilled professionals with smart technology to get your claims paid faster and keep your cash flowing. No more drowning in administrative tasks – we handle that so you can focus on your patients.
We don’t believe in one-size-fits-all solutions. Every practice is unique, and our services flex to fit your needs. With clear data and practical insights, you’ll always know where your money is and where it’s going. Choose a partner who cares about your success as much as you do.

Client's Feedback

Outstanding service! There is no delay in processing of our claims and they are always processed appropriately.

Highly professional team. They have greatly enhanced the cash inflow of the business.

Billing has always been a problematic area for me until I came across this– perfect billing without any issues.

Their expertise in compliance is invaluable. No more costly penalties!
Specialized Healthcare Billing Solutions for Every Medical Practice
Every medical specialty has its billing quirks – we know them all. From pediatrics to cardiology, our team works alongside your practice to fine-tune the billing process. Let us handle the claims while you handle the care.
Frequently Asked Questions
What benefits can I expect from outsourced medical billing services?
You’ll see fewer errors, better compliance, and more time for patient care. Plus, our professional approach typically leads to better collections and healthier revenue.
What services do you include with medical billing outsourcing?
We cover it all – claims processing, EDI enrollment, denial management, patient billing, revenue cycle optimization, compliance monitoring, and clear financial reporting.
How do you structure your pricing?
We tailor our pricing to your specific needs and complexity. Give us a call or fill out our web form for a custom quote that fits your practice.
What specialties do you support at MedLife?
We work with a wide range of specialties including primary care, cardiology, neurology, dermatology, urology, pediatrics, and many more. Each gets the specialized attention it deserves.







